Vaping
Vaping and Electronic Nicotine Delivery Systems (ENDS)
Vaping Overview
Electronic vapor products or electronic nicotine delivery systems (ENDS) are referred to by a variety of names including e-cigarettes or e-cigs, vapes, vape or hookah pens, mods, tank systems, Pod systems or disposables. Many are made to look like regular cigarettes, cigars, or pipes, while others resemble pens, USB sticks, or other everyday items. Liquid used in these products typically contains nicotine, flavorings, and other chemicals and is aerosolized by a battery-powered heating element in the device. Users inhale this aerosol into their lungs. ENDS can also be used to deliver cannabis and other drugs. Use of these products is commonly referred to as vaping, ‘hitting’ or ’ripping’. Many ENDS devices are rechargeable and refillable, allowing users to create their own ‘e-juice’ flavor and vary the nicotine levels. E-liquids may have a high level of nicotine which can be poisonous, especially for young children. Though flavors were restricted in cartridge-based devices by the Food and Drug Administration (FDA) in 2020, there are thousands of liquid or ‘e-juice’ flavors available, many of which are candy or fruit-flavored and appealing to youth.

Graphic Courtesy of Centers for Disease Control and Prevention
Most ENDS consist of four components: a cartridge or reservoir (which holds a liquid solution), a heating element, a power source (usually a lithium battery), and a mouthpiece. Currently, the most widely used devices are pod-based and disposable such as Elf Bar, Puff Bar, or Juul.
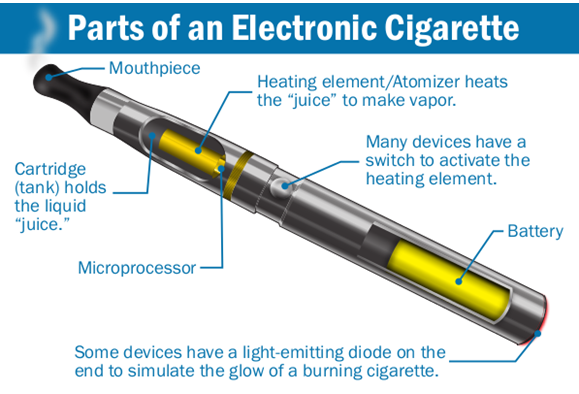
Graphic courtesy of Wikimedia.com
Health Risks
Nicotine is a highly addictive substance and is not safe for youth, pregnant people, or their developing babies. Nicotine can harm brain development, impact behavior, and effect respiratory health.
The aerosol inhaled and exhaled from ENDS is not harmless. It can contain nicotine, heavy metals, ultrafine particles, and other toxic substances.
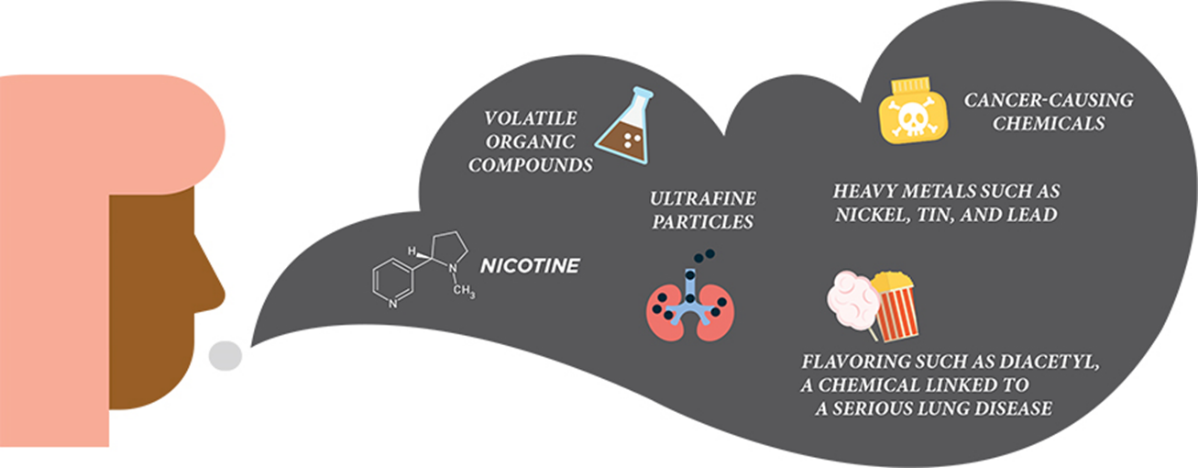
Graphic courtesy of the Centers for Disease Control and Prevention
In 2019, a nationwide outbreak of E-Cigarette or Vaping Associated Lung Injury (EVALI) was investigated. Vitamin E acetate, an additive to THC-containing e-cigarette or vaping products was strongly associated with the outbreak. The Centers for Disease Control and Prevention (CDC) provided a 2023 update on the status and characteristics of the outbreak.
More research is needed to determine if ENDS are an effective tobacco cessation tool for adults. They are not an FDA approved aid for quitting.
Environmental Risks
ENDS contain hazardous components that impact the environment including batteries, microplastics, and chemicals like nicotine. Improper disposal can pollute soil, water, and harm wildlife. Defective vaping device batteries have also caused some fires and explosions, a few of which have resulted in serious injuries.
Read more about how tobacco harms the environment.
CT Data Trends
ENDS are the most prevalent form of tobacco product used by Connecticut high school youth. In 2021, more than 1 in 10 high school students reported past 30-day use of vaping products compared to just over 1 in 100 reported past 30-day use of cigarettes.
About 13% of adults have tried ENDS at least once in their lifetime, including nearly 23% of young adults. Nearly 30% of adults who vape also smoke combustible cigarettes.
Visit Stats & Reports to learn more about tobacco use in Connecticut and view state-specific data.
Resources
General
- CT DPH Vaping Factsheet
- CT DPH Flavored Tobacco Products Factsheet
- CT DPH Menthol Flavored Tobacco Products Factsheet
- CT DPH Nicotine Information Factsheet
- CT Tobacco Laws
Parents
- Supports for Parents | VapeFreeCT: a health-department sponsored website that provides resources and tips for parents to help keep kids vape- and smoke-free.
- E-cigarettes and Youth: What Parents Need to Know | CDC
- Parent Resources | Truth Initiative
Healthcare Professionals
- Online Provider Referral | Commit To Quit
- E-Cigarettes and Youth: What Health Care Providers Need to Know | CDC
- Clinical Practice Tools and Resources | American Academy of Pediatrics
School Professionals
- CT DPH Safe Disposal for Electronic Nicotine Delivery Systems (ENDS) Factsheet
- Empower Vape-Free Youth | CDC
- Alternatives to Suspension | Live Tobacco Free
Cessation
- CT DPH Tobacco Use Cessation Factsheet
- VapeFreeCT: Quit resources for youth and young adults ages 13-24 including a free text message cessation program.
- CommitToQuit: Quit resources for adults and youth as young as 13 years old including 24/7 chat and phone support.
- CT Cessation Program Directory: A list of statewide in-person cessation programs.

